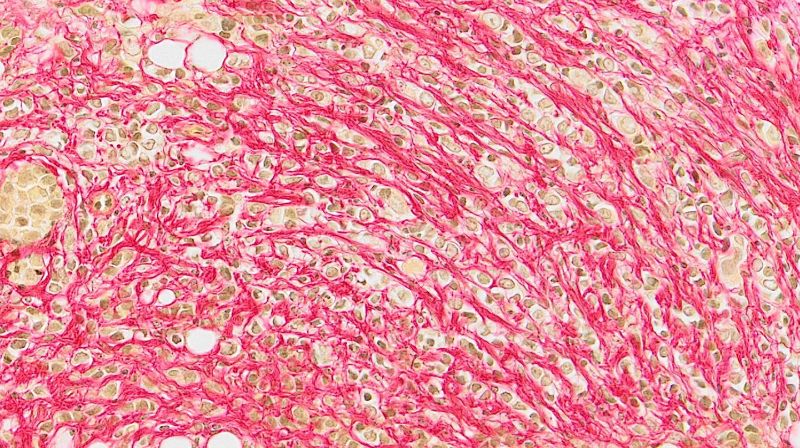
Scientists model a peculiar type of breast cancer
Invasive lobular carcinoma (ILC) is a type of breast cancer that begins in the milk-producing glands (lobules) of the breast. It covers 10-15% of all breast cancer cases, has a high risk of late recurrence, unique metastatic sites, high sensitivity to hormones, unpredictable responses to therapies, unique histopathology, distinctive biology, and resists chemotherapy. More than 90% of ILC tumors also contain estrogen receptors, meaning that they can receive hormone signals from the body e.g. estradiol, that can spur their growth and metastasis.
Despite all this, ILC is relatively understudied compared to other breast cancers, and as a result, there have been very few models developed to study it. The reason is the lower incidence of ILC in general, but also because ILC tumors don’t lend themselves to growth in culture or in mice, which is key to developing models.
Now, scientists at EPFL’s have successfully overcome the limitations of ILC and have developed a xenograft model for it that simulates the tumor with high accuracy. The scientists, led by EPFL researcher George Sflomos, at the laboratory of Professor Cathrin Brisken grafted two ILC-derived metastatic breast cancer cell lines as well as freshly resected ILC tumors from patients directly into the milk ducts of mice which are immune deficient. The study is now published in EMBO Molecular Medicine.
The approach allowed the researchers to develop a series of in vivo models of lobular breast cancer. It is particularly important that these experimental ILC tumors retain estrogen receptor expression, as well as their responsiveness to estradiol that ILC tumors typically show. “The samples preserve the histomorphological aspects, and the peculiar metastatic patterns of ILC. The findings are particularly important for studying ILC metastasis which is primarily responsible for ILC cancer-related mortality,” says George Sflomos, first author of the study.
The model tumors also revealed some secrets of ILC biology. They appear to have similar peculiarities in the extracellular matrix such as their intrinsic ability to produce elastin, collagens, and the collagen-modifying enzyme LOXL1. So, when the researchers blocked all LOX enzymes, they saw a decrease in primary tumor growth, metastasis, and estrogen receptor signaling. “LOXL1 proved essential for in vivo tumor progression, which suggests that targeting the ILC tumor’s microenvironment can be a promising therapeutic approach that open up new horizons on the biology of the disease that would benefit ILC patients,” says Sflomos.
“This model provides us with the first in‐depth insights into the most common of the breast cancer special types estrogen receptor-positive breast cancer subtype,” says Cathrin Brisken. “This experimental modeling of ILC will help identify molecular mechanisms specific to the disease, and discover new therapeutic targets in the near future.”