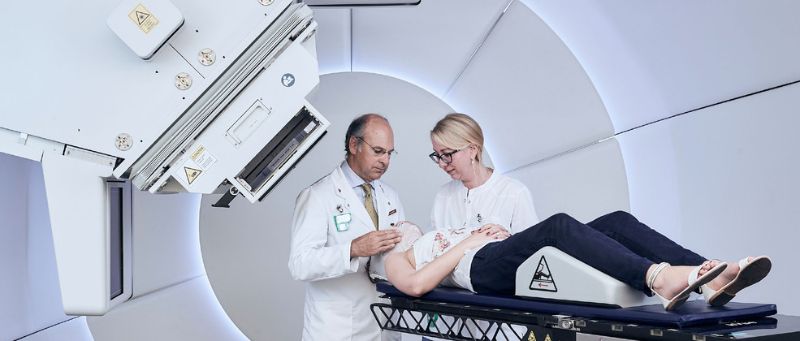
Proton therapy: a success story that started 25 years ago
It was Monday, and the team was gathered in the control room at the Center for Proton Therapy. "We were huddled together, peering anxiously at the monitor relaying images from the treatment room," recalls Martin Grossmann, a physicist with the Center for Proton Therapy (CPT) at PSI. Back in the 1990s he was part of a team of 15 researchers led by Hans Blattmann, Eros Pedroni and Gudrun Goitein developing a new technology for treating cancer patients: spot scanning, also known as pencil beam scanning.
The moment of truth came on 25 November 1996: a human patient lay waiting in the treatment room. The 62-year old man from the Canton of Lucerne had malignant skin cancer that had already formed metastases in his brain. The purpose of the intervention was to irradiate these rogue metastases using the new technique.
Despite meticulous preparations, the team was nervous. "You can treat as many plastic dolls or models as much as you want, but when you have a live patient lying there, it’s a totally different experience," says the medical physicist Tony Lomax, one of the development team. That Monday he helped to place the patient in the exact position for the proton beams to precisely target the area of the body to be irradiated. The tolerance was a question of millimetres: "A proton beam is like an extremely sharp tool," Martin Grossmann stresses. "There is no room for error."
A huge success
The team of specialists ensured that the technology functioned smoothly and eventually everyone was able to breathe a sigh of relief: the treatment had gone exactly as planned – just as Martin Grossmann and Tony Lomax had expected. "We were all firmly convinced we had mastered the technology. We made a huge effort to ensure that everything was absolutely safe for the patient," Grossmann notes.
In the following year, CPT moved on to successfully treat several other cancer patients. The medical world was initially sceptical – the technology seemed too unmanageable at the time. During the ten years up to 2008, the Paul Scherrer Institute was the only facility in the world to use this technique. Since then, spot scanning has become established worldwide and now ranks as standard procedure for proton therapy.
Eradicating the tumour
"Proton therapy has completely revolutionised the battle against cancer," says Damien Weber, senior clinician and head of CPT. In proton therapy, a proton beam – a concentrated beam of rapidly moving, charged particles – kills cancer cells by destroying their DNA. Conventional radiation therapy works on the same principle, but uses X-rays rather than protons to destroy the malignant cells.
Protons have a big advantage over more energy-intense radiation, however, Weber goes on to explain. They can be precisely targeted to the specific area of the body, where they unleash their destructive effect. "Undesirable side-effects caused by radiation are therefore much less common, which makes the method especially suitable for children, but also for tumours in particularly sensitive or inaccessible areas of the body." Tumours in the region of the head, neck or spine are typical candidates for treatment.
For a long time the medical profession favoured the scattering technique for proton therapy. With this method, the proton beam is spread out and, using an individually tailored metal aperture plate, filtered to match its shape to the size and contour of the tumour. Today this is still the preferred method for treating eye tumours. Not so for deeper-seated tumours.
"We already knew the spot scanning technique would offer a lot of advantages here," says Tony Lomax. The malignant tissue is scanned with the proton beam – "a bit like sketching its outline with a pencil," Lomax explains. Or rather rubbing it out with an eraser. The exact position of the tumour is determined beforehand with the help of imaging techniques such a CT or MRI scan, and the proton beam programmed so that precisely the right amount of charged particles is targeted at the areas to be treated.
PSI’s location advantage
Looking behind the scenes at the Center for Proton Therapy, it soon becomes clear why this technology could only have been developed at PSI rather than in a hospital, for example. The radiation unit (called a gantry) itself is the size of a large truck, and even bigger and more complex equipment is needed to generate the proton beams and deliver them to the gantry.
"Here we are actually working with applied accelerator physics," says Martin Grossmann. “We need measurement devices that control the path of the beam. We need ultrafast electronics to control the magnets used. And above all we need highly qualified people with the skills to build such a machine. These can’t be found in a hospital.”
The concept of spot scanning first arose in Japan. "But our team at CPT was brave enough to say at the time: let’s actually try using that technique," Grossmann. The resulting success story has been a blessing for cancer patients over the past 25 years – and beyond.