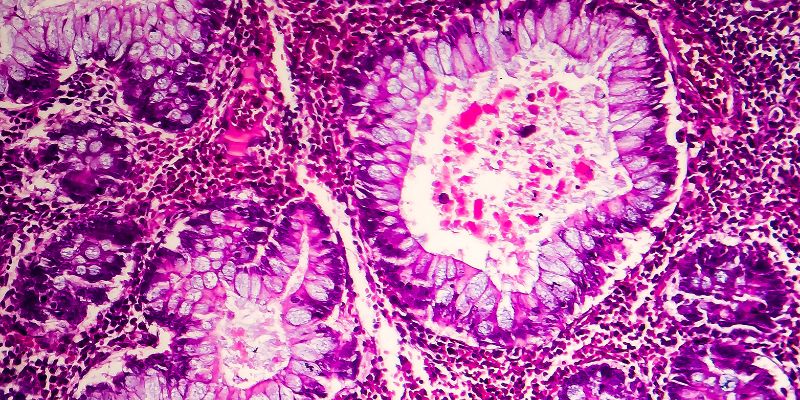
Exploring the architecture of tumours
The fact that every tumour is different makes cancer treatment one of the most complex areas of medicine. A degenerate cancer cell grows into a mosaic of cell populations that continuously acquire new mutations. And each of these cell populations – or “clones” – can react differently to treatment.
Modern treatment approaches target those cell populations that contribute significantly to tumour growth. Doctors take tumour tissue samples and determine the relative size of the clones and their specific mutations by means of DNA sequencing.
However, it is often unclear whether and why a certain cell population becomes established in a tumour, making it difficult to predict the further development of the cancer and choose the right treatment accordingly.
Computer model shows tumour development
An international research team led by Niko Beerenwinkel, professor in the Department of Biosystems at ETH Zurich in Basel, has now shown that tissue architecture is a crucial factor in determining how cell populations spread in different types of cancer.
The researchers simulated tumour development using a computer model that, unlike previous models, takes into account not only the mutations, but also the way in which the cancer cells are arranged in the affected tissue and how they spread. Their results have been published in the journal Nature Ecology and Evolution.
“Cell populations in tumours compete with each other for limited resources, such as space, nutrients and oxygen,” explains Robert Noble, the study’s lead author. This means that the question of whether a new mutation confers a survival advantage to a cell population depends on how it interacts with neighbouring cell populations.
Cancer cells are in permanent competition
In the case of blood cancer, for example, there are up to 100,000 blood stem cells in the bone marrow in form a large, uniform poolinteracting community. A degenerate stem cell with a mutation that confers a survival advantage can rapidly establish itself in this cell pool.
In contrast, the cells involved in the development of colon cancer are located individed into small niches that are separated by microscopic folds of the intestinal wall. Due to the highly compartmentalised nature of the habitat, cancer cells with beneficial mutations are slow to spread.
The theory that the spatial structure of tissue influences tumour evolution has existed in cancer research for some time. However, the new study is the first to systematically investigate this aspect. The computer model of the ETH researchers shows the tissue-specific spread of the mutated cell populations for different types of cancer.
Simulations agree with architecture of real tumours
The newly developed computer model shows the tissue-specific spread of the mutated cell populations for different types of cancer. For each type of cancer, the researchers ran thousands of simulations and compared the results with with spatially resolved DNA sequencing data from real human tumour specimens. The predictions of the computer model agree with the clinical data.
“Our results show that the particular spatial structure of each tumour must be taken into account in order to obtain an accurate picture of the processes,” says Beerenwinkel.
The study also provides a blueprint for a new generation of patient-specific models in cancer diagnostics. Noble, who now leads a group at City, University of London, says: “In future, doctors might be able to use these models to better predict whether a particular tumour will respond to treatment.”